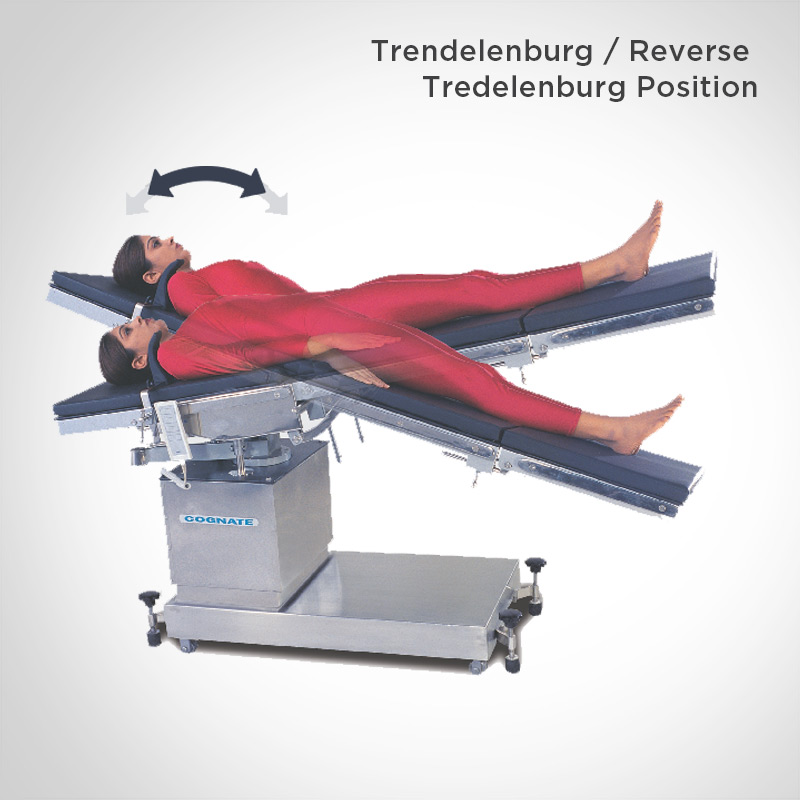
Trendelenburg is currently recommended by the American Society of Anesthesiologists as the optimal position for central line insertion, when clinically appropriate and feasible, to facilitate cannulation and prevent the occurrence of air embolisms. Potential adverse effects include increases in intracranial pressure, decreased lung expansion/lung volumes caused by pushing the diaphragm upward, baroreceptor effects promoting a false sensation that blood flow improved which leads to vasodilation, and a decreased response to the hypotensive state (Shammas & Clark, 2007). The controversy lies in whether blood moving from the extremities to the central part of the body contributes to hemodynamic stability and whether there are harmful effects that outweigh benefits. Also known as autotransfusion, Trendelenburg became common practice in various healthcare settings such as emergency rooms, operating rooms, post-anesthesia care units, and critical care. During World War I, the position was utilized in the treatment of shock to increase circulation to the heart, increase cardiac output, and improve blood flow to the vital organs (Shammas & Clark, 2007). Friedrich Trendelenburg, a surgeon, pioneered this technique to gain better access to pelvic organs during operative procedures. The origins of Trendelenburg trace back to the late 1800s, when Dr. However, researchers found that the use of Trendelenburg does not improve blood pressure and shock and instead, could have detrimental effects on specific patient populations. I quickly integrated Trendelenburg into my everyday practice. It certainly made logical sense and seemed to work, at least transiently. 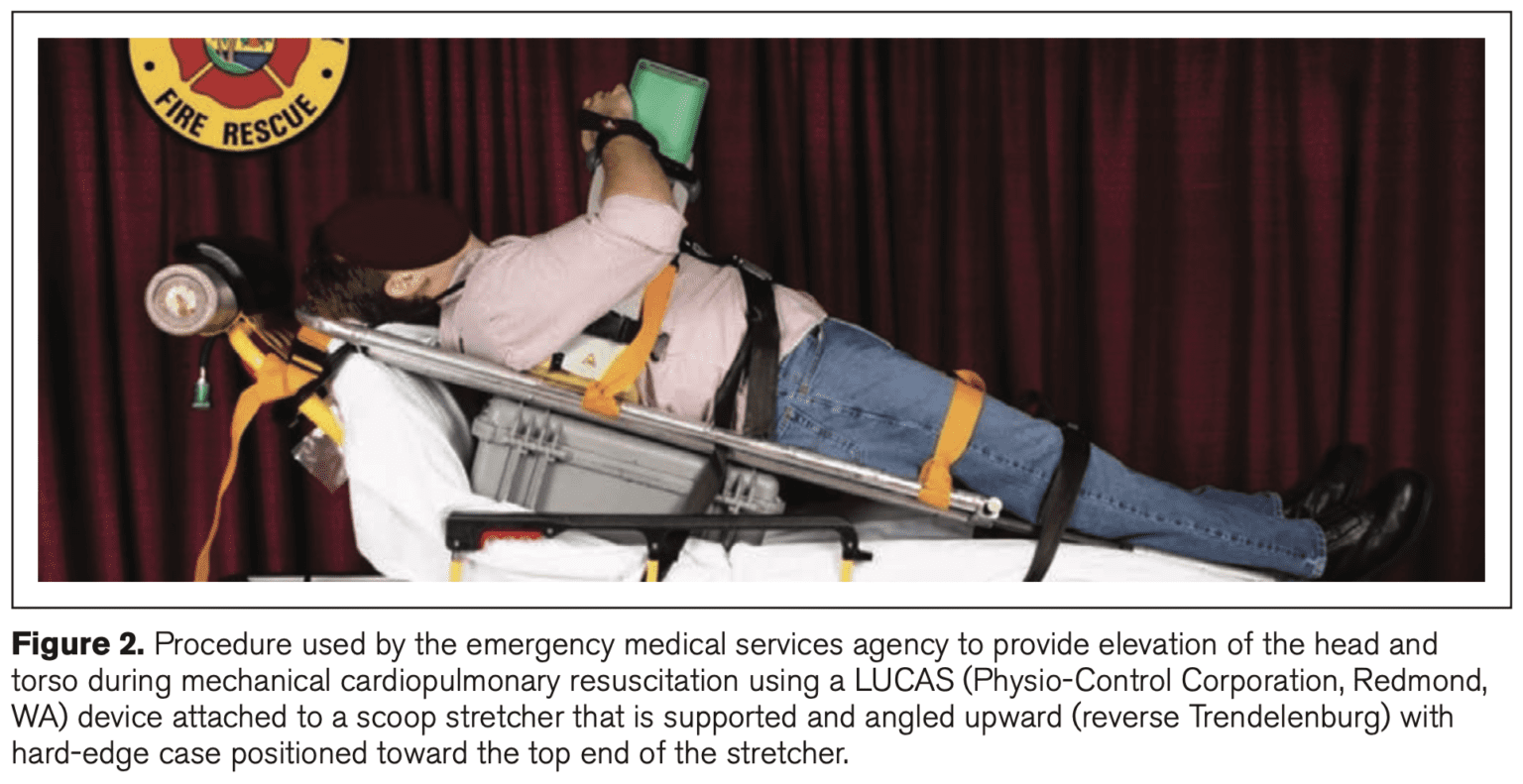
She explained that lowering the patient’s head and elevating the legs above the heart helped to move blood from the lower extremities to the heart, brain and other vital organs. When I first started my nursing career in the early 1990s, I remember watching my preceptor in the critical care unit reflexively place her patient in the Trendelenburg position during episodes of acute hypotension and shock. Facing Ethical Challenges with Strength and Compassion.Establishing Yourself as a Professional and Developing Leadership Skills.Ensuring Patient & Family Centered Care.Developing Critical Thinking Skills and Fostering Clinical Judgement.Alteplase Injection for Acute Ischemic Events.Lippincott Clinical Conferences On Demand.Continuing Education Bundle for Nurse Educators.Lippincott NursingCenter’s Critical Care Insider.Lippincott NursingCenter’s Career Advisor.COVID-19 2022 Update: The Nursing Workforce.An Unforeseen Path from Critical Care Nurse to Editor-in-Chief of American Journal of Nursing.When Nurses Speak, People Listen: An Interview with Pat Patton.Psychological Safety and Learner Engagement: A Conversation with Dr.Fostering a Safe and Healthy Work Environment through Competency-Informed Staffing.Innovation in Nursing Education Practice: A Conversation with Linda Honan.Clinical Judgment: The Doing that Happens after Critical Thinking.Debriefing: It Should Always Be About the Learner.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
